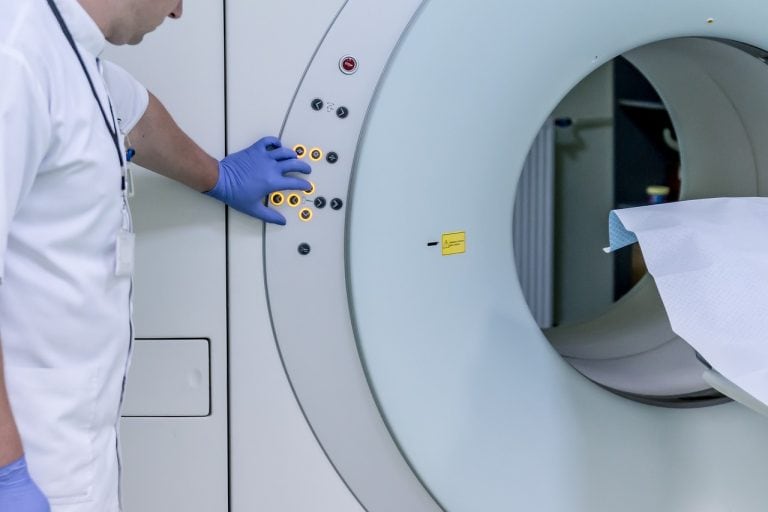
Medical imaging guides many clinical choices and mistakes in those images can have serious consequences. Artificial intelligence is changing how scans are processed and how subtle patterns are picked out from noise and artefact. Machine learning models can flag anomalies verify measurements and reduce routine slip ups by staff working under pressure. The sections that …
How Can AI Prevent Errors in Imaging Results? Learn More

Medical imaging guides many clinical choices and mistakes in those images can have serious consequences. Artificial intelligence is changing how scans are processed and how subtle patterns are picked out from noise and artefact.
Machine learning models can flag anomalies verify measurements and reduce routine slip ups by staff working under pressure. The sections that follow outline concrete ways AI reduces errors across acquisition processing interpretation and reporting.
AI For Noise Reduction
Raw image noise can mask tiny lesions or create false signals that mislead readers. Deep learning models trained on paired noisy and clean scans learn to remove noise while keeping edges and texture that matter for diagnosis.
When noise is lower radiologists can see subtle contrast changes and automated tools that detect lesions make fewer false calls. The result is clearer data with fewer spurious findings and a lower chance that a treatable problem will be missed.
Automated Image Segmentation
Accurate borders around organs and lesions matter for diagnosis staging and follow up. AI segmentation tools can trace boundaries automatically and produce consistent masks even when anatomy is distorted by disease or prior surgery.
For readers who want to understand how these tools perform in real clinical environments it can be useful to review success stories from imaging leaders who have already integrated similar systems into daily workflows.
That consistency cuts down on variation between readers and helps measurements match from one visit to the next. When segmentations are offered as overlays the human reader can accept tweak or reject them quickly saving time and reducing random error.
Standardizing Acquisition And Protocols
Variation in how scans are acquired creates a lot of needless confusion for downstream interpretation. Smart systems monitor acquisition parameters in real time and alert technologists if settings fall outside expected ranges so re scans can be done when needed.
Consistent input leads to more consistent outputs and models tuned to stable protocols perform better on day to day cases. A uniform approach shrinks one major source of error that comes from mismatched techniques across different sites or machines.
Quality Control And Artifact Detection
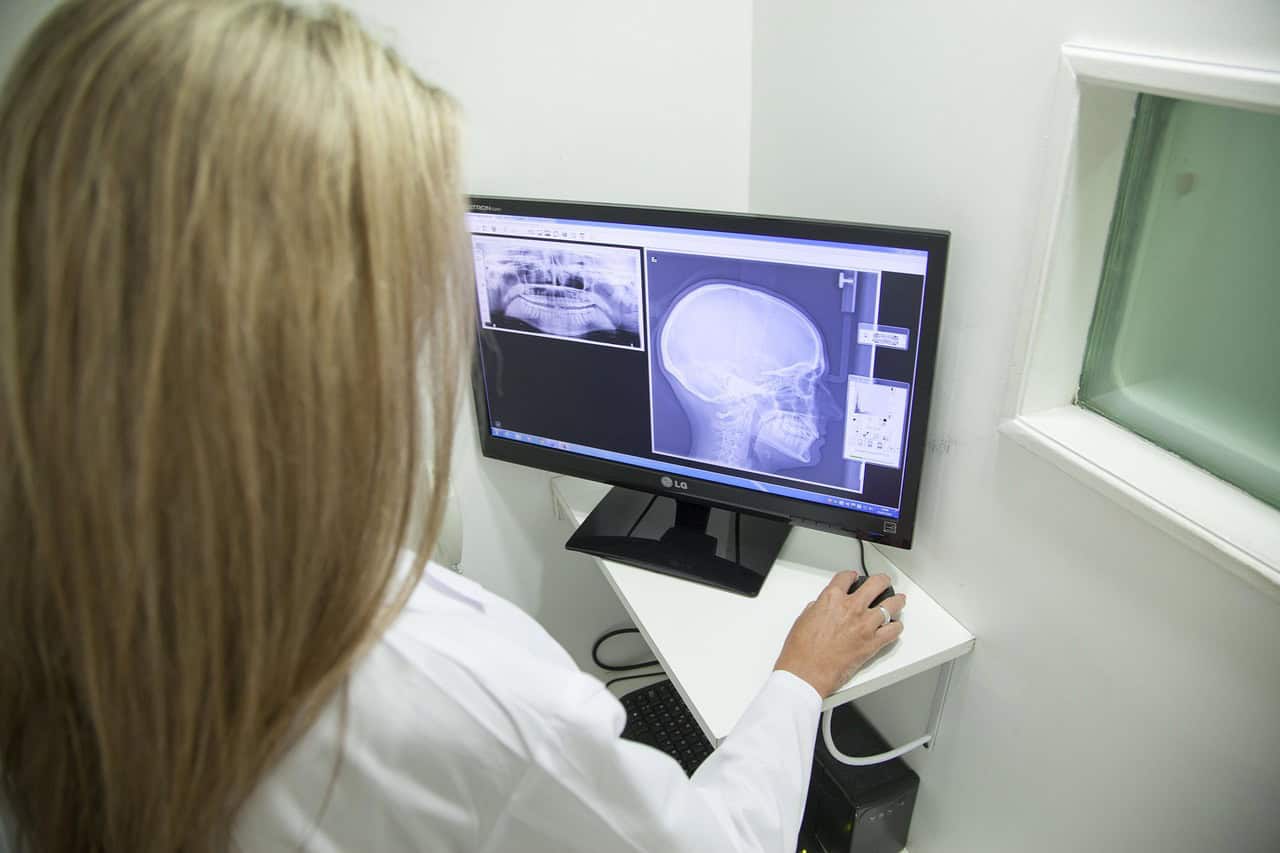
Motion metallic objects and truncation can wreck an otherwise useful study. AI tools trained to spot those artifacts flag affected images and suggest repeat scanning or alternative views right away.
Automated checks cut down the time wasted chasing bad data and reduce the risk of a report that relies on flawed images. Fewer corrupted studies mean fewer misreads and less downstream testing driven by false alarms.
Decision Support And Case Prioritization
Not every scan requires the same urgency level and some critical findings are subtle until the last moment. AI can triage studies by highlighting probable acute events so they move up the reading list and catch attention sooner.
When risk is flagged early clinicians respond faster and patient outcomes benefit from timelier action. The system acts as a second pair of eyes that nudges human readers toward what needs focus first.
Automated Measurements And Quantification
Manual measurements are prone to variability depending on the reader and the method used. Automated quantitative tools produce repeatable metrics for things like tumor size ejection fraction or plaque burden and they apply the same rules every time.
That repeatability helps teams compare values across visits and reduces confusion when different clinicians contribute to care. Consistent numbers also make it easier to spot real change rather than measurement noise.
Confidence Scores And Explainability
A raw label alone can breed overconfidence or doubt in the clinician who reads the study. Introducing confidence scores and visual explanations such as heat maps gives context about why a model reached a decision and how certain it is.
When users see both the prediction and the degree of certainty they blend machine output with their own judgement more effectively. Clear indications of uncertainty tend to curb blind trust and lead to more careful review of ambiguous cases.
Continuous Learning And Feedback Loops
Performance on historical test sets does not guarantee stability in the clinic over time. Systems that accept curated feedback from experts and that update models on validated new data adapt to subtle shifts in patient mix equipment or practice patterns.
A loop where humans correct algorithm errors and the algorithm learns from those corrections reduces repeat mistakes. Ongoing monitoring with periodic retraining helps keep error rates down as conditions change.
Integration Into Workflow And Reporting
Isolated tools create friction and that friction breeds mistakes when people cut corners to save time. Seamless integration into picture archiving and reporting systems means AI outputs appear where readers already work making adoption simpler.
Structured outputs such as pre filled measurements annotations and suggested text speed up report generation and reduce transcription errors. Embedding AI into familiar workflows encourages consistent use and less special handling that can introduce variability.
Regulatory Records And Audit Trails
Documentation about how a decision was reached matters when a result is questioned later on. Systems that keep timestamped logs of model versions inputs outputs and any human edits create a traceable audit trail for quality review.
Such records support peer review credentialing and incident analysis and help teams identify recurring gaps that need teaching. When the past is easy to inspect it becomes simpler to correct patterns that otherwise persist unnoticed.